Welcome | Logout
Introduction
The following Portal Training Guide is the official training manual for the UHC portal. All new portal users should review the sections of the guide that align with their job function. The guide lists all the steps to using the functionality within the portal. As updates are made to the portal, this guide will be updated for users to review and familiarize themselves with any new changes to the functionality..
Getting Started
Logging In
As a part of the onboarding process, you will receive login information. If you are a user who requires access, please contact the Super Admin user within your organization to grant you access to UHC portal.
Forgotten Password
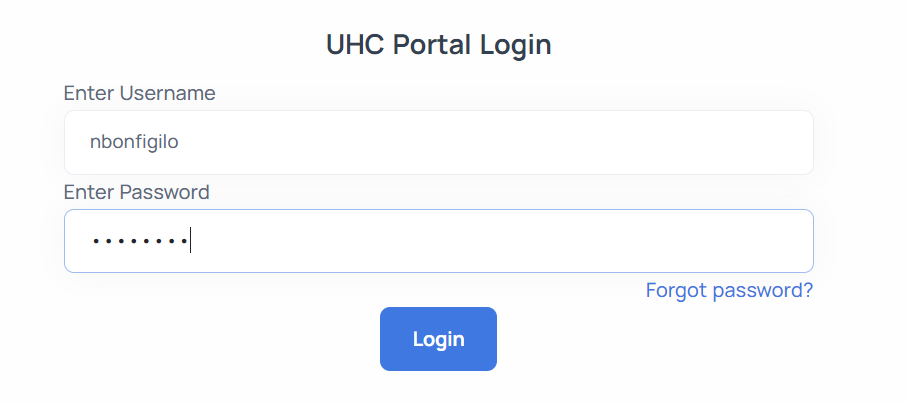
In the event you forget your password, you can reset your password by loading the login page, here, and clicking the "Forgot password?" button. Once redirected, simply follow the prompts in the dialogue boxes and the system will direct you to set a new password. Only you will know this password so be sure to save it some place safe. Once you receive your new password, proceed to enter your credentials into the login box depicted below.
Landing Page
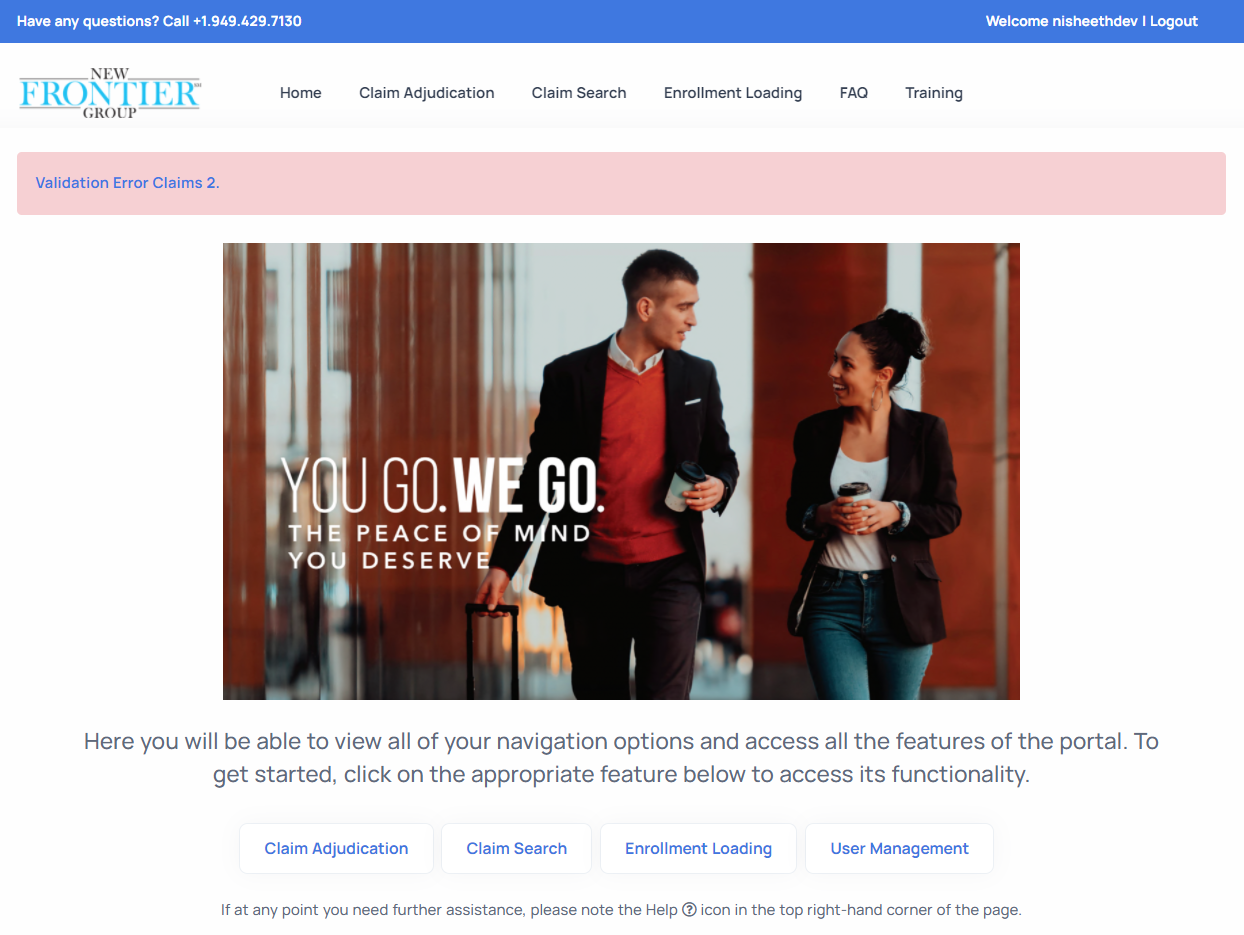
After logging in, you will be brought to the UHC Portal Landing Page. The landing page allows you to navigate within the UHC Portal and its different functions using either the navigation ribbon or the selectable options buttons.
It is important to note that only users with a Super Admin role will have access to the User Management feature depicted above. Every organization is assigned a Super Admin user
Claim Adjudicaiton
Accessing Claim Adjudication
You will typically begin your day by accessing the Claim Adjudication tool. To start, simply click on the Claim Adjudication button either from the navigation ribbon or from the selectable option below the graphic.

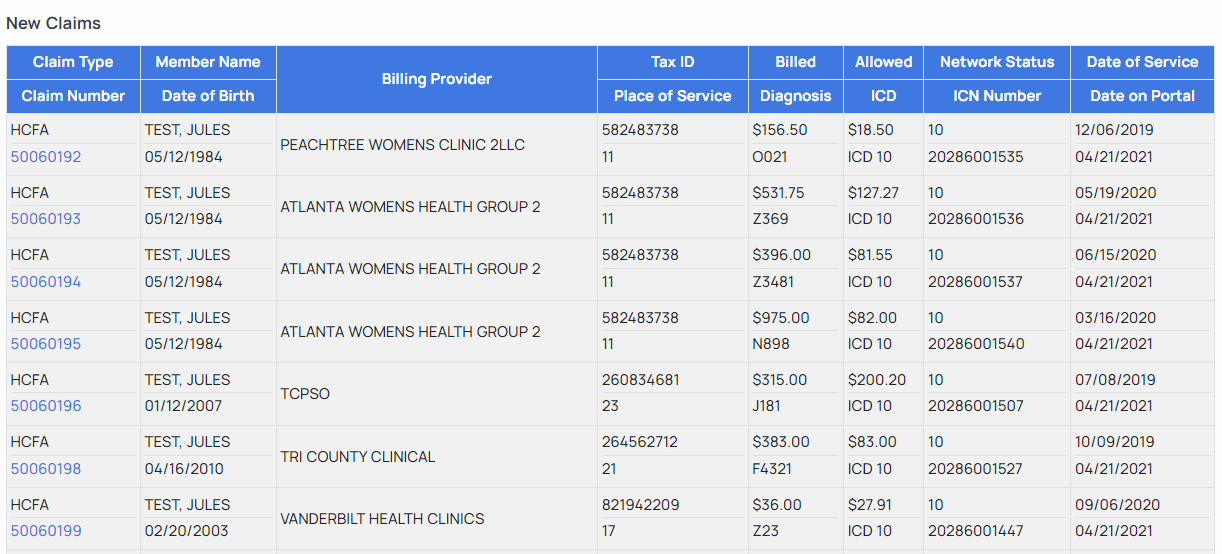
After navigating to the Claim Adjudication tool, you will be presented with the following page. The tool will list out the claims in sub queues based on status. To begin, click on the Claim ID for the claim you wish to adjudicate as depicted below.
Sub Queue Definitions
| CLAIM ADJUDICATION SUB QUEUES | |
|---|---|
| NEW | This queue contains new claims that have yet to be worked by a claims processor. New Frontier Group recommends that Claims processors work the claims in this queue starting with the oldest claims first to ensure that claims to do not age. |
| SUBMITTED | This queue contains claims that have already been worked and submitted by a claims processor. These claims can be reviewed to see prior adjudication submitted but are not typically the priority. |
| VALIDATION ERROR | This queue contains claims that were previously worked on by a processor but after submitting the adjudication a validation error was detected. These claims should be prioritized before new claims so that they can be corrected and resubmitted as quickly as possible to offset aging. |
Adjudicating Claims
Claim Level
After you click on the Claim ID of the claim you wish to adjudicate, the Claim Adjudication workbench will be displayed as depicted below. This is where you will apply the benefits to the claim.
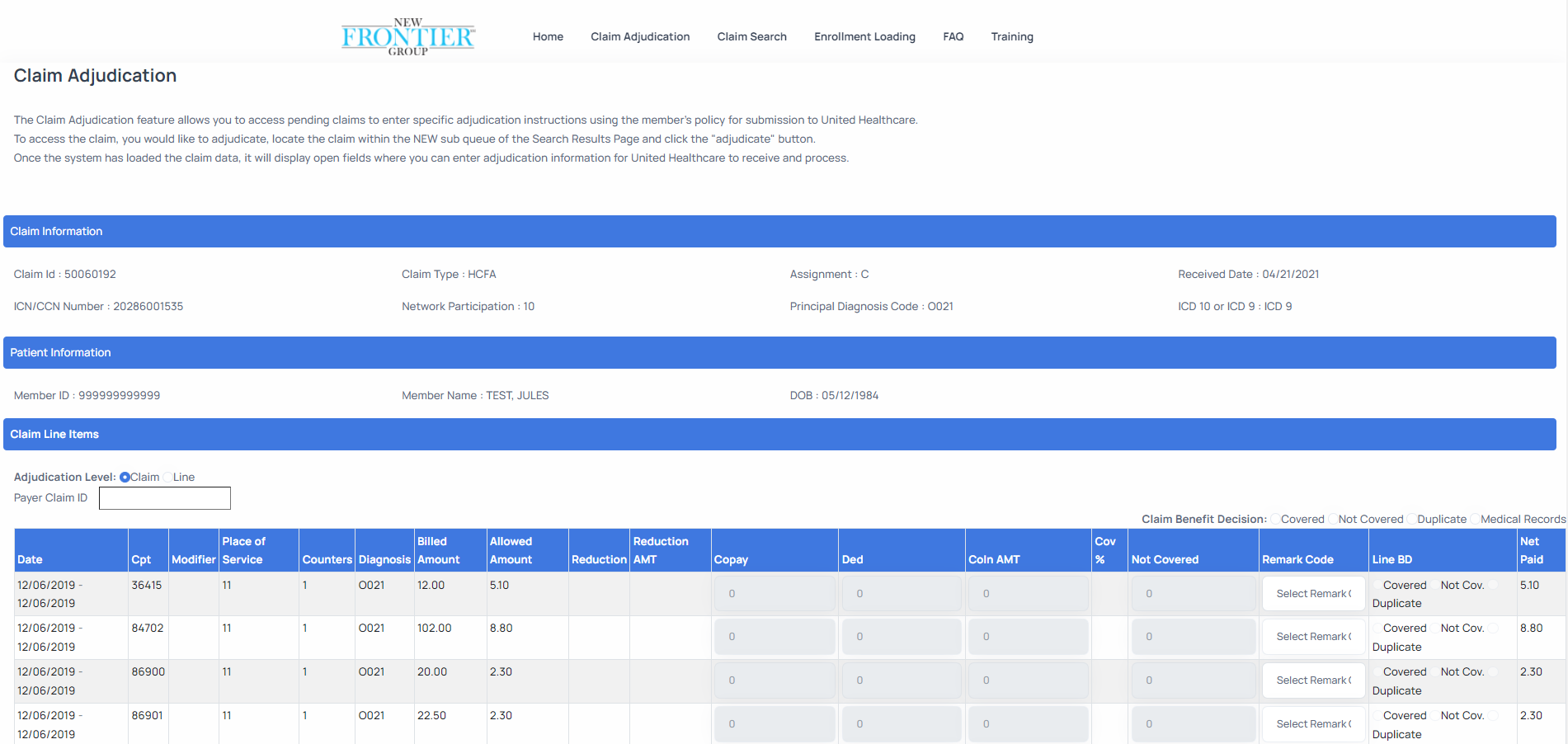
To optimize the adjudication process New Frontier Group recommends that you follow the sequence below when applying benefits.
- Start by selecting the Adjudication level you would like to apply benefits.
- Next Select the benefit decision you wish to apply to the claim.
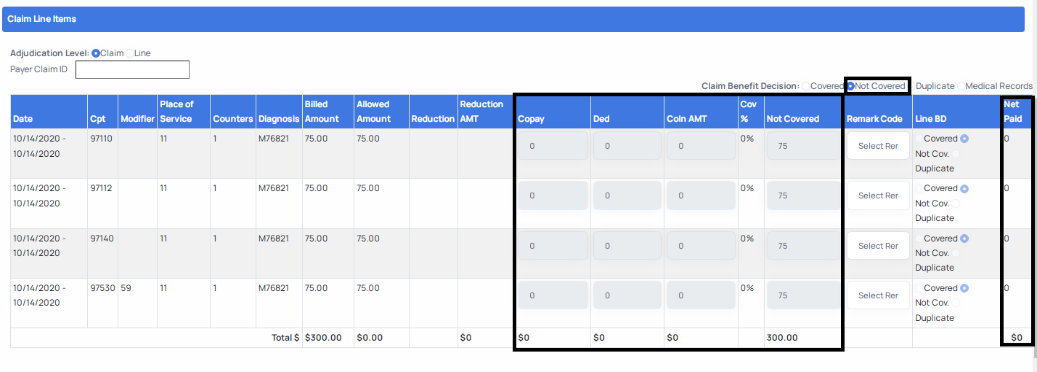
- If you select any benefit decision other than Covered the Claim Adjudication page will auto calibrate the disposition of the adjudication fields for you to ensure that they are correct. After clicking the benefit decision, you will see the values for the fields change to align with you benefit decision selection. It is important to note that the highlighted fields below will auto calibrate, but you must select a remark code from the drop- down menu for every line of the claim. See a depiction of this below for the benefit decisions other than covered.
a. Claim level Adjudication: This means you intend to apply the benefits at claim level only. This type of adjudication is more typical for Facility claims.
b. Line Level adjudication: This means that you intend to apply the benefits at line level. This type of adjudication is more typical for Professional claims.
a. Covered: This is the most typical benefit decision. If you select covered benefit decision, it means that the members policy requires that a payment be made to the provider that is greater than $0.00.

b. Not covered: This is the benefit decision you would select if you intend to deny the claim or line of claim. It is important to note that if you select this benefit decision you MUST indicate one of the highlighted remark codes from the list below or you will not be able to submit the claim successfully. The remark code is required to provide context for the denied charges when the claim is received by United.

When using the Not Covered benefit decision please select one of the remark codes in black below.

c. If after reviewing the charges you determine that they have been processed previously then you can select the Duplicate benefit decision. It is Important to note that when selecting the Duplicate benefit decision at either claim or line level you must also select the "05" remark code and ensure it appears in the Remark Code field.

d. Medical records: In some cases, you will require additional information before finalizing the claim adjudication. By selecting the Medical Records option, you will be placing a request with United to solicit and obtain the medical records for the claim you are working on. It is important to note that the medical records benefit decision is ONLY selectable at claim level. If you select this option, it will apply to all lines of the claim.

a. Not Covered benefit decision
b. Duplicate benefit decision
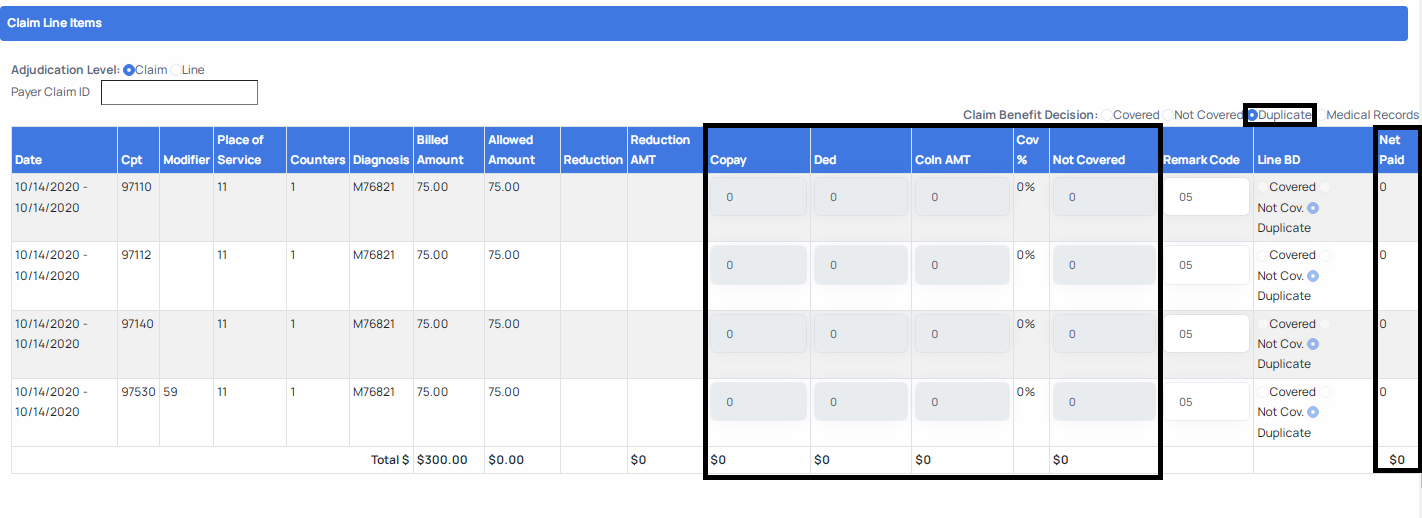
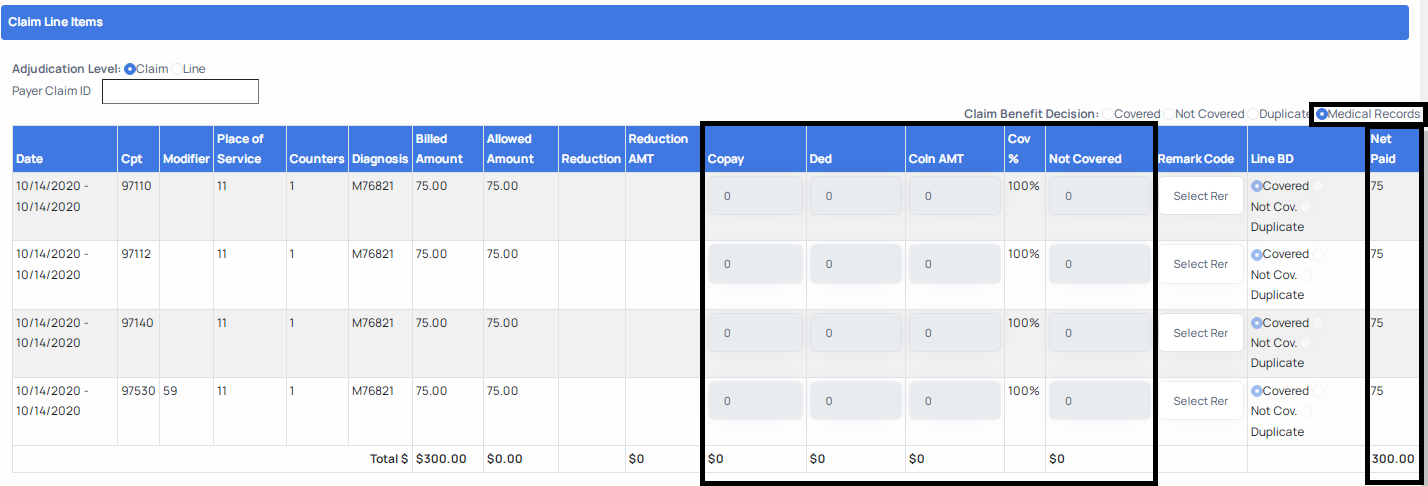
c. Medical Records decision
Line Level
- If you select Line Level adjudication, you must ensure that prior to submitting your adjudication to click the Update Lines button depicted below. Using this button will ensure the system sums up the individual line level values so that you claim adjudication matches at line and claim level. It is important to note that if at any point you wish to restart the adjudication process, simply click the Reset Values button shown below to clear all previous values.
- The Covered Benefit decision allows you to indicate a net paid amount greater than zero. Use this benefit decision when you are adjudicating claims in a way where a payment must be made to the provider. To use the Covered benefit decision, follow the process outlined below.
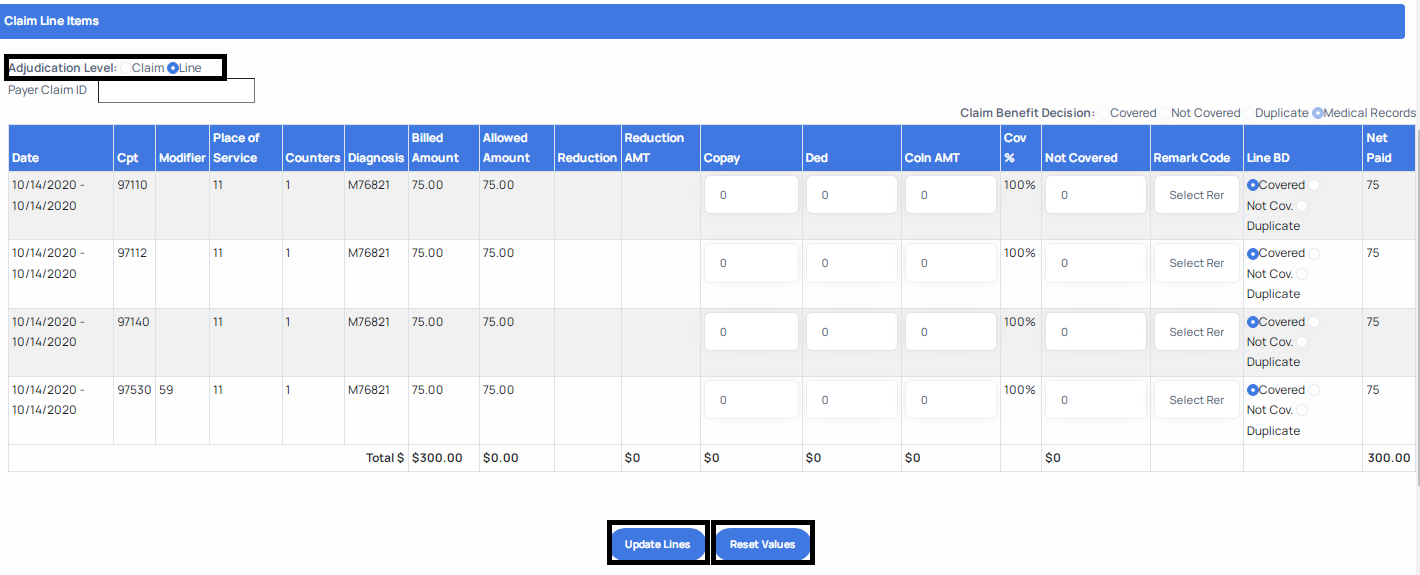
a. Start by selecting the adjudication level: Claim or Line level
b. If adjudicating at claim level, select the Covered benefit decision from the Claim level options depicted.

c. If you are adjudicating at line level, you must select the Covered benefit decision for all the individual lines it applies to.
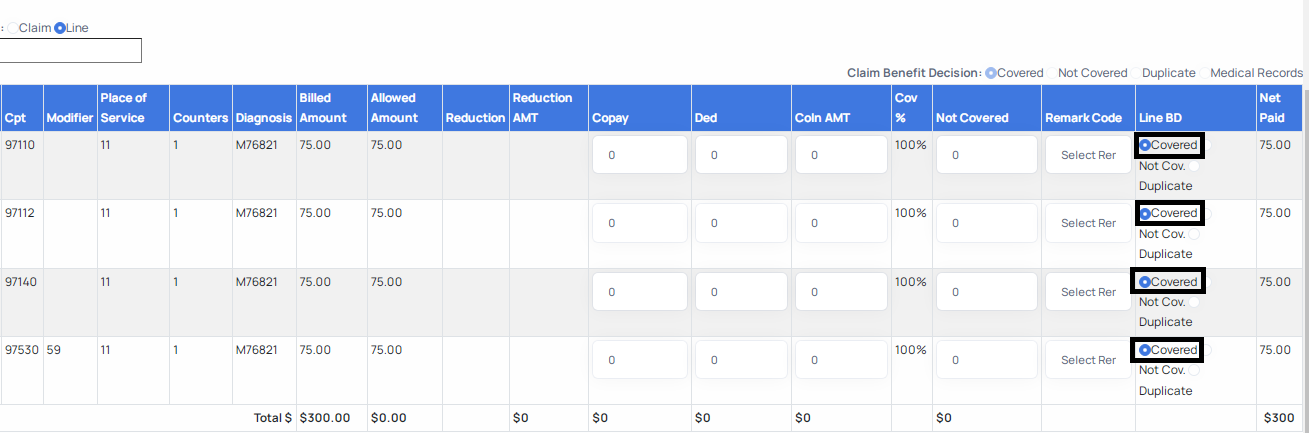
d. After you have designated the benefit decision either at claim or line level, next begin to indicate the specific adjudication values that apply to the claim.
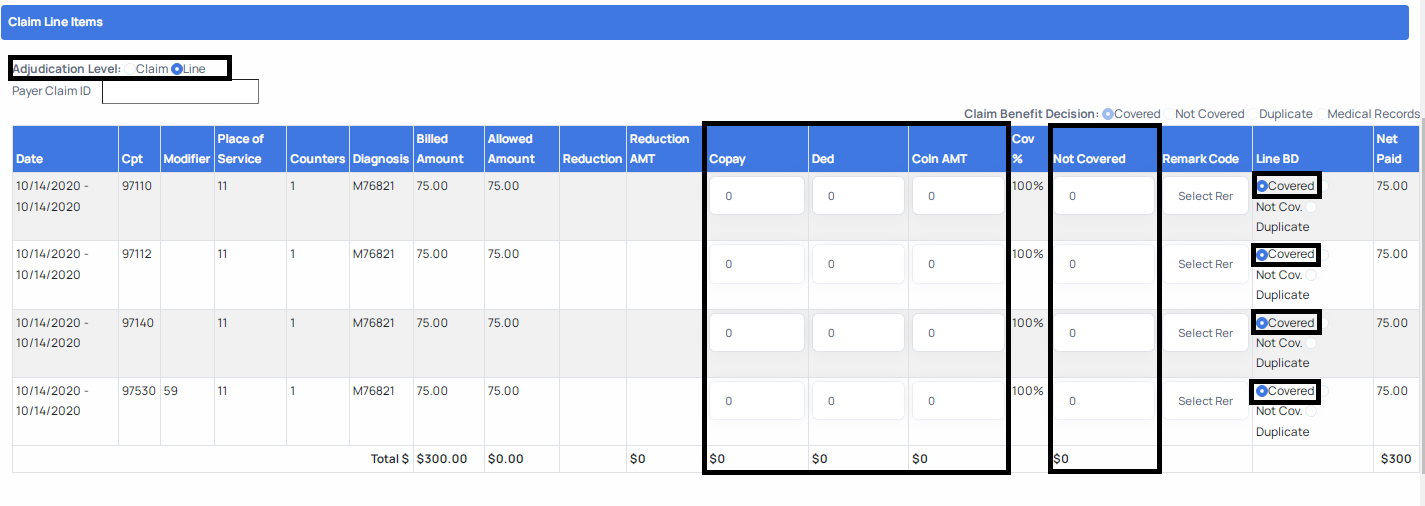
e. To enter either Deductible, Co-pay, Co-insurance, or Not Covered amounts when adjudicating at line level, simply access the fields depicted below to enter these values. It is important to note that while adjudicating claims at line level, you must click the Update Lines button before clicking Submit in order to successfully submit your adjudication. This button ensures that the system summates all the line level values you have entered to populate the sum totals at claim level.
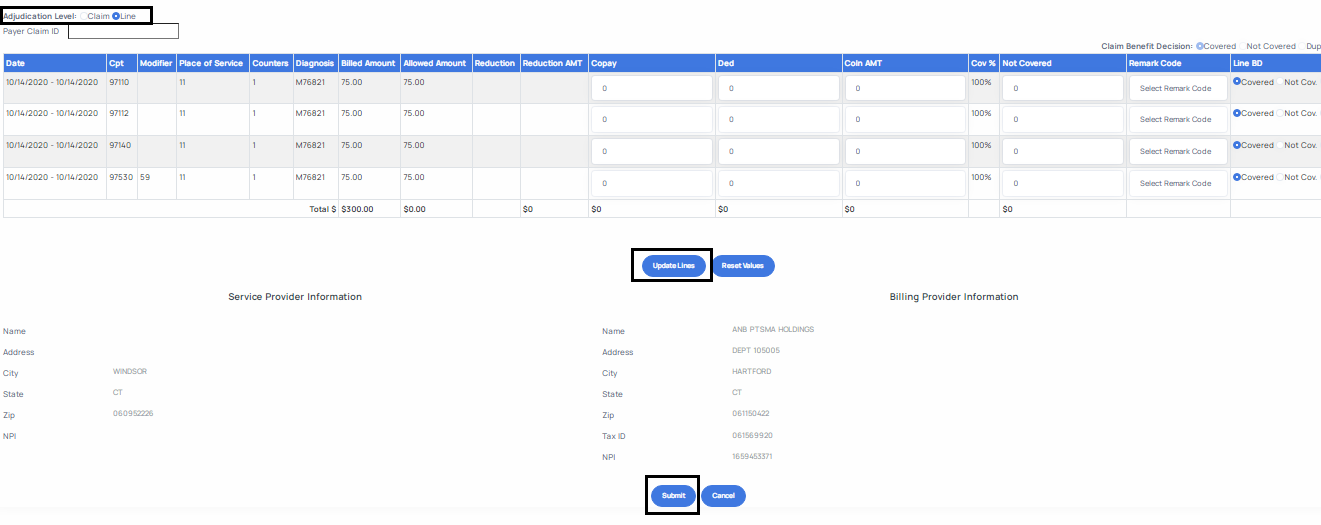
f. If you are adjudicating a claim at claim level, you will simply enter the claim level total for these values in the fields depicted below.
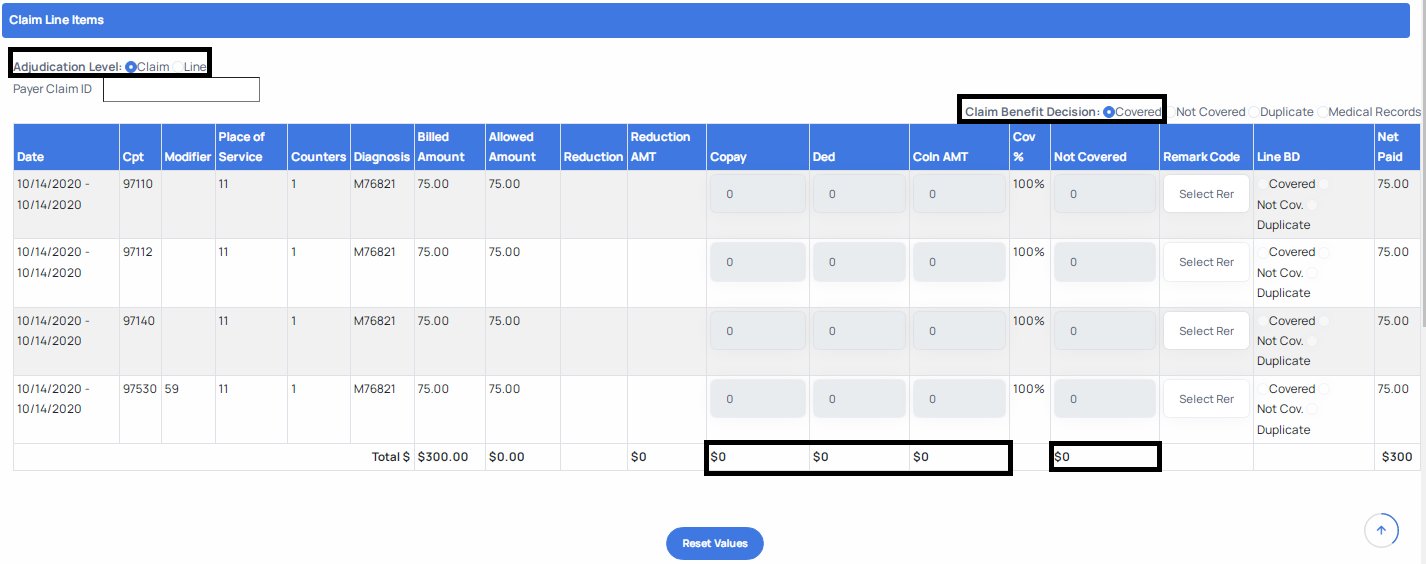
Validation Errors
When you click the Submit button after adjudicating a claim, the system will subject your claim adjudication to the following validation rules depicted in the chart below.
| Rule | How to check for this | Message to display |
|---|---|---|
| Line level Not covered amount must be accompanied by a Remark code selection | If line level Not Covered > 0 then line Remark code cannot be blank | Validation Error: You must enter a line level remark code for line with not covered amount greater than zero. Please select a Not covered Remark code at line level to explain the charges being denied. |
| Claim level Not covered amount must be accompanied by a Remark code selection | If Claim level Not Covered > 0 then claim level Remark code cannot be blank | Validation Error: You must enter a Claim level remark code for Claim with not covered amount greater than zero. Please select a Not covered Remark code at claim level to explain the charges being denied. |
| Line with ICES reduction must have Approved benefit decision | If Reduction Reason = ICES, then live level benefit decision MUST equal Covered | Validation Error: You must select the Covered benefit decision at line for any line of the claim that has an ICES reduction. Please select the Covered Benefit decision for any line with an ICES reduction reason before re- submitting this claim. |
| Total of line level Copay deductible and Coinsurance cannot exceed the allowed amount | Sum of line level values Copay + Deductible + Coinsurance less than or equal to Allowed amount | Validation Error: The line level sum of the out-of-pocket amounts (Copay, Deductible and Coinsurance) must be less than or equal to the line level allowed amount. Please reduce the line level out of pocket amounts before re-submitting this claim. |
| Total of Claim level Copay deductible and Coinsurance cannot exceed the allowed amount | Sum of Claim level values Copay + Deductible + Coinsurance less than or equal to Claim level Allowed amount | Validation Error: The Claim level sum of the out-of-pocket amounts (Copay, Deductible and Coinsurance) must be less than or equal to the Claim level allowed amount. Please reduce the claim level out of pocket amounts at claim level before re-submitting this claim. |
| Line Level Not Covered Amount Cannot exceed Line Level billed charges | If line level allowed is <= Line level Billed charges, THEN Line level Not covered amount less than or equal to Line level Billed charges | Validation Error: The line level Not covered amount cannot exceed billed charges if the line level Allowed amount is less than or equal to billed charges. Please reduce the line level. Not covered amount before re-submitting the adjudication. |
| Claims Level Not Covered Amount Cannot exceed Claim Level billed charges | If Claim level allowed is <= Claim level Billed charges, THEN Claim level Not covered amount <= Claim level Billed charges | Validation Error: The Claim level Not covered amount cannot exceed Claim Level billed charges if the claim level Allowed amount is less than or equal to Claim Level billed charges. Please reduce the Claim level Not covered amount before re-submitting the adjudication. |
| Update lines button must be clicked before submitting claim adjudication if line level adjudication was applied. | If Adjudication Level = Line level AND If the sum of the line level Copay amounts > Claim level Copay OR If the sum of the line level Deductible amounts > Claim level Deductible OR If the sum of the line level Coinsurance amounts > Claim level Coinsurance OR If the sum of the line level Not covered amounts > Claim level Not covered Then cause claim to fail and display error message | Validation Error: You must click the "Update Lines" button before clicking the "Submit" button if you selected Adjudication Level as Line Level. |
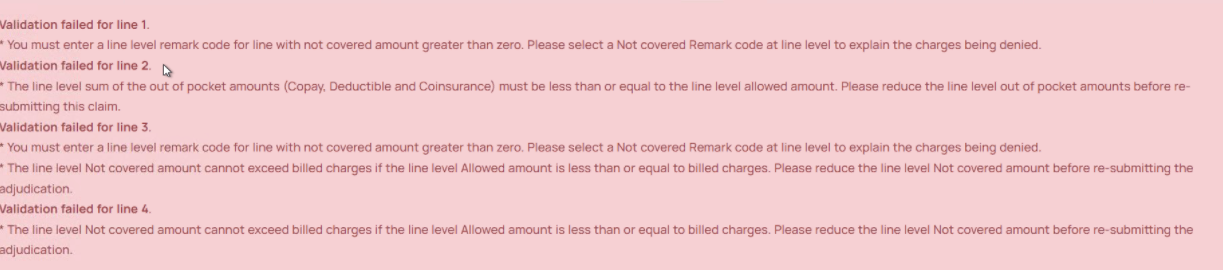
- If the system detects any of these errors above after you have clicked the submit button, it will cause a validation error which will prevent the claim from being successfully submitted. The system will display a message in the format and syntax depicted below. If such an error message is displayed, then you will need to review the specific error indicated using the line number reference as a guide.
- Once you have made the necessary corrections outlined by the validation error message, please proceed to click the submit button again to submit your claim adjudication.
- Now that your adjudication has been successfully submitted two things will happen:
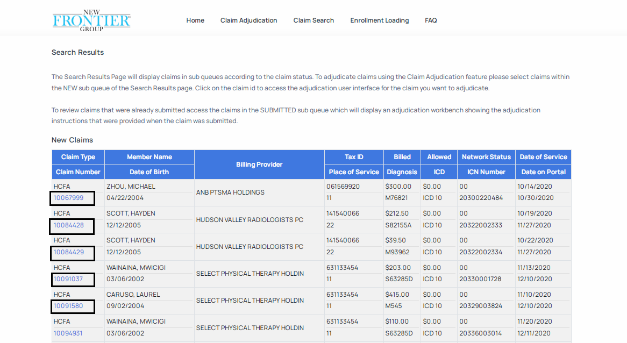
- You will be routed back to the Search Results screen depicting the Validation Error and NEW CLAIMS sub queues so that you can select another claim to adjudicate.
- The claim you submitted will have its status updated to SUBMITTED and will now appear in the SUBMITTED sub queue on the Claim Search Results Page.
Definitions for Adjudication Fields
| Sr. Number | Field | Definition |
|---|---|---|
| 1 | Allowed Amount | The Allowable Amount is the amount after Reduction amounts (COB/iCES/Duplicate/R&C) have been subtracted. The Allowable Amount is then the basis for the Benefit Determination. |
| 3 | Benefit Decision | The Benefit Decision will indicate if the outcome of benefit determination on the claim and/or line is Covered, Not Covered, or Duplicate.
UHCG uses the Benefit Decision on the claim and/or line to process the claim.
Note: For Professional Claims, UHCG accepts Benefit Decisions at both the Claim Level and Line Level. For Institutional Claims, UHCG accepts Benefit Decisions at the Claim Level only. UHCG supports following Benefit Decisions via EDI: a. Benefit Decision of Covered - '1' b. Benefit Decision of Not Covered - '2' c. Benefit Decision of Duplicate - '3' d. Benefit Decision of Medical Records - '4' |
| 4 | Coinsurance Amount | Coinsurance is the portion of covered health care costs the covered person is financially responsible for, usually according to a fixed percentage. Coinsurance is often applied, according to a fixed percentage, after a Deductible and/or Co-Payment requirements are met. |
| 5 | Copayment | A cost-sharing arrangement in which a covered person pays a specified amount for a specified service, such as $20 for an office visit. The covered person is responsible for payment at the time the health care is rendered. Typical co-payments are fixed or variable flat amounts for physician office visits, prescriptions, or hospital services. Some co-payments are referred to as coinsurance, with the distinguishing characteristics that co-payments are flat or variable dollar amounts and coinsurance is a defined percentage of the charges for services rendered. |
| 7 | Coverage Percentage | Coverage Percentage is the portion of covered health care costs the plan is financially responsible for, usually according to a fixed percentage. Coverage Percentage is often applied, according to a fixed percentage, after a Deductible and/or Co-Payment requirements are met. UHCG expects Coverage Percentage to be a whole number between 0 and 100. |
| 9 | Deductible Amount | Deductible is a portion of the benefits, under a policy that a covered person must satisfy before any reimbursement occurs. |
| 10 | Diagnostic Report | The Diagnostic Report captures the Error messages at the Claim and Line Level while processing Outbound and Inbound EDI Files. | 13 | Medical Record Request | Medical Record Request is a process to request the medical documentation in order to adjudicate the claim. The request is made via sending the EDI2 claim with Benefit Decision as 4 and then the Business team send the record manually. |
| 14 | Net Paid Amount | Net Paid Amount is the amount that will be paid to the provider. Net Paid Amount Equals Allowed Amount minus Net Patient Responsibility. |
| 15 | Net Patient Responsibility | Net Patient Responsibility is the amount the patient or
his/her representative(s) is responsible for paying to the
provider: Net Patient Responsibility Equals Copay + Coinsurance + Deductible + Not Covered Amount + R&C Reduction |
| 16 | Not Covered Amount | The Not Covered Amount includes Benefit Limits/Sub Limits, Exclusions (Specific conditions or circumstances for which the policy or plan will not provide coverage reimbursement), and Plan Maximums. |
Claim Search
Accessing Claim Search
The claim search feature allows you to search for a specific claim or a subset of claims that have the same attribute. To use the Claim Search feature, simply follow the instructions below.- Click on Claim Search from either the feature options on the landing page or from the option in the navigation ribbon as depicted below.
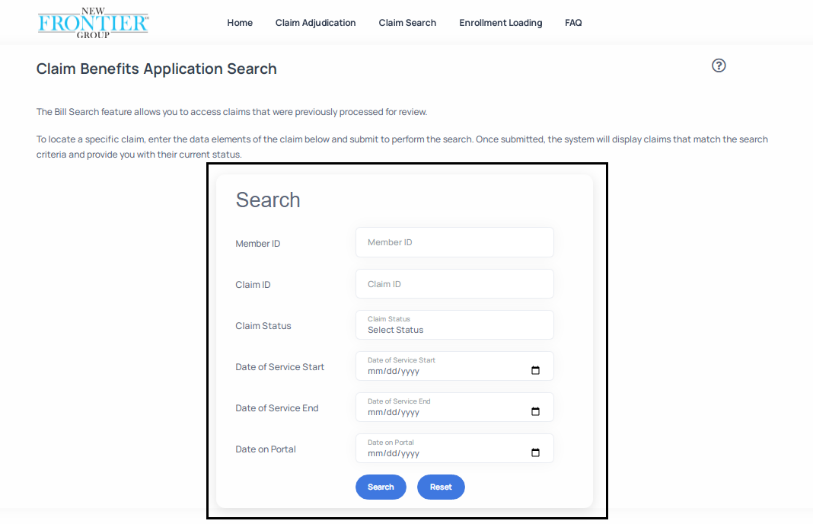
- Next, the Claim Search page will load, and display the data entry fields depicted below.
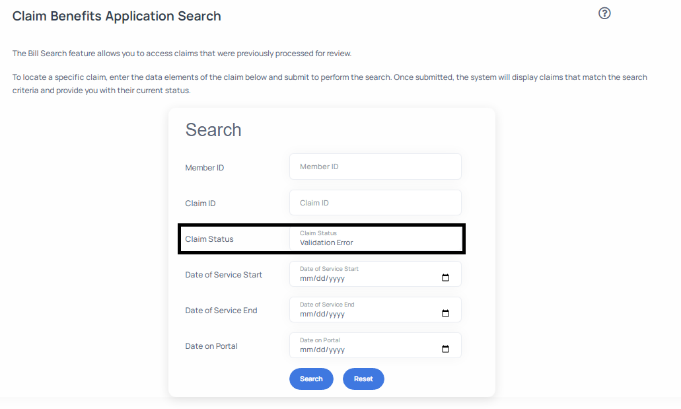
- Determine the criteria that you would like to use to search for claims. In this case a criterion of Claims Status = Validation Error was used. It is important to note that you can also choose to run the search with all fields empty. This open search will display all Validation Error and New Claims in their sub queues.
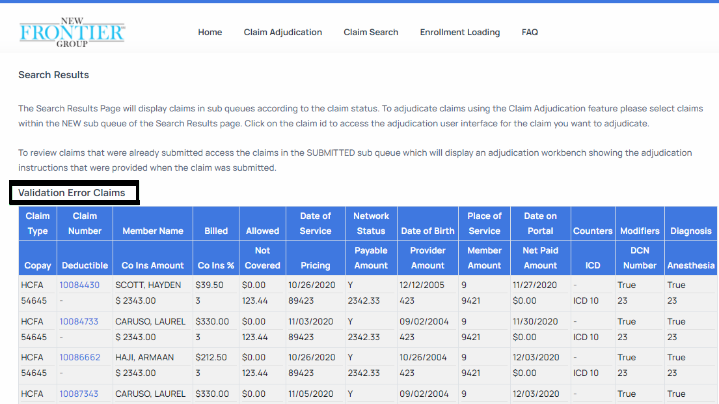
- After you have entered your search criteria click the Search button to execute the search. This will display the Search Results page as depicted below. This page will list out the subset of claims that match the criteria entered.
- To select the claim you wish to view or adjudicate, simply click on the Claim ID for that claim as depicted below.
Enrollment Loading
Accessing Enrollment Adjudication
The UHC Portal has an Enrollment Loading tool which you can use to submit either single enrollments or BK35 enrollment files to United Healthcare for loading and processing.
- To use this feature, go to the landing page and simply click on the Enrollment Loading option from the navigation ribbon at the top of the page or the buttons below the image.
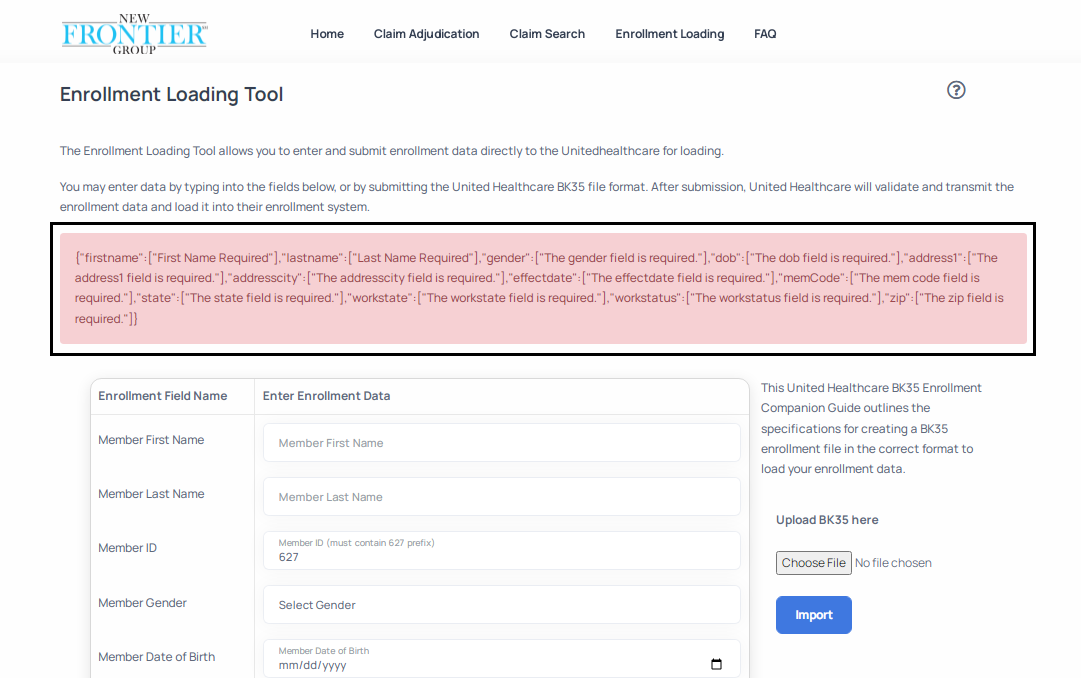
- This will load the Enrollment Loading Page depicted below.
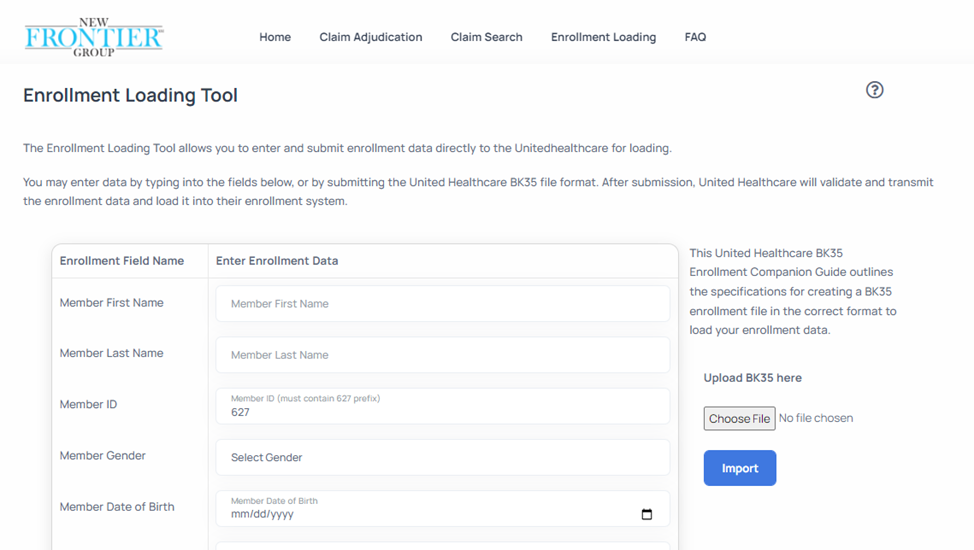
Single Form Enrollment
- The single enrollment loading tool will allow you to submit a single enrollment at a time and should be used when you want to enroll a member on the fly.
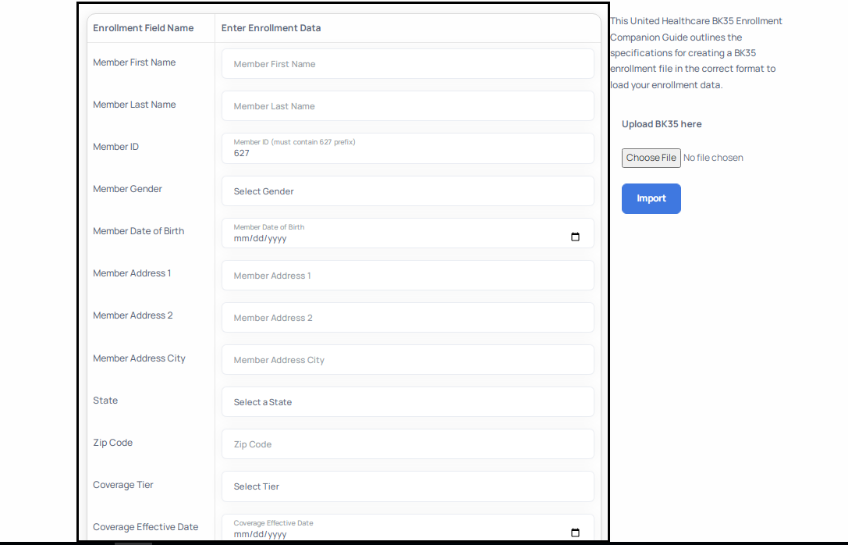
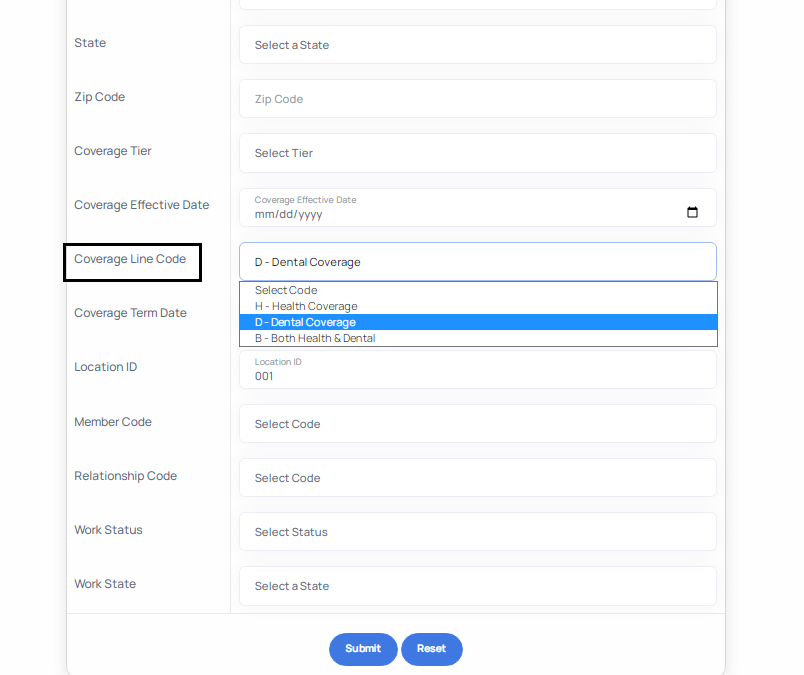
- To use the single enrollment form, begin by populating the data entry fields on the left side of the screen as depicted below.
- As you type in information, you will notice that for some fields there is a drop-down list that limits the data that can be entered in that field. This has been done so that you can select from valid data to ensure successful submission.
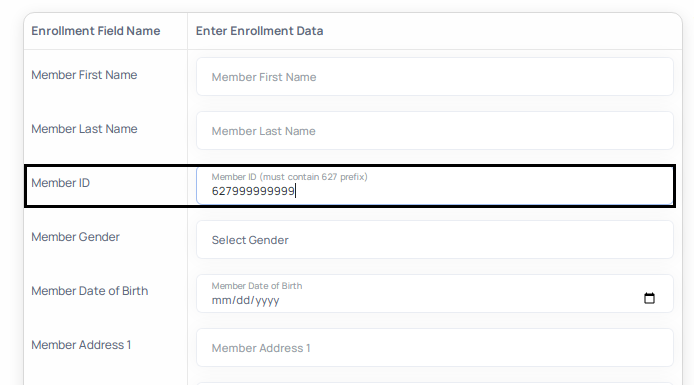
- When populating the Member ID number that you want to assign for the member, it is critically important to ensure the number submitted is within the range for your class code.
- If you fail to populate a data element the system will display an error message like the one depicted below.
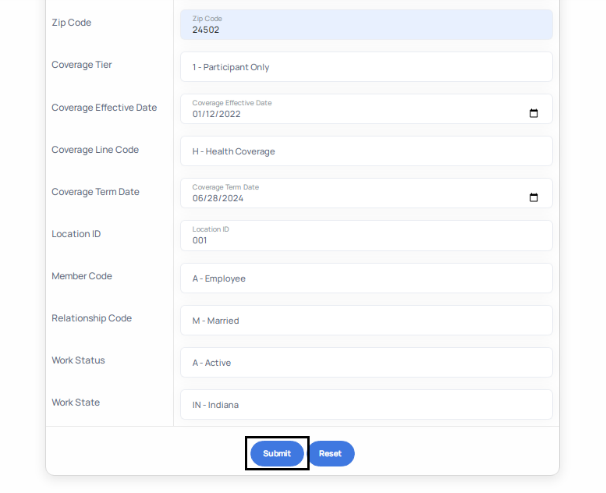
- You must correct the error or populate the blank field in order to submit your data successfully. After making the necessary corrections, click the submit button to successfully submit the single form enrollment data. Once submitted, your enrollment data is sent directly to United Healthcare to be loaded.
BK-35 File Enrollment
- The BK35 loading portion of the Enrollment Loading tool is available for submission of enrollment files.
- To use the BK35 submission tool you will need to use the guide below to prepare the BK35 file in a structurally sound format.
- BK35 Enrollment File
- See below for the rules governing the data elements for each individual column of data
- Once you have prepared your file save it on your desktop or in the documents folder on your local machine.
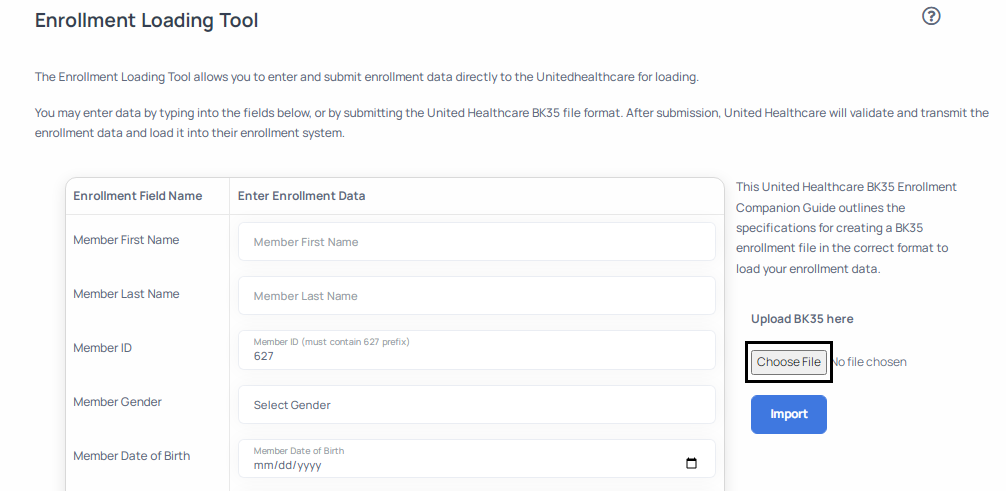
- Click on the choose file button depicted below.
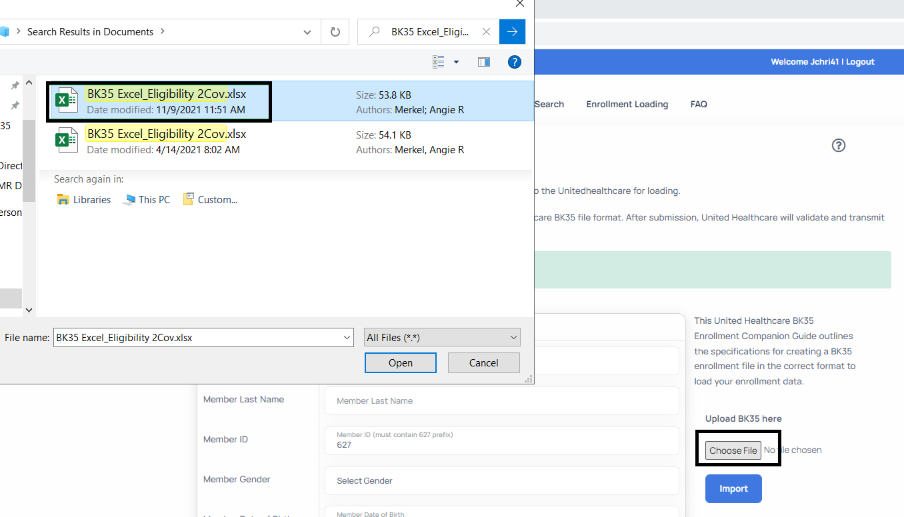
- This will allow you to select the file you saved in step 4 above. Select the BK35 file and click open.
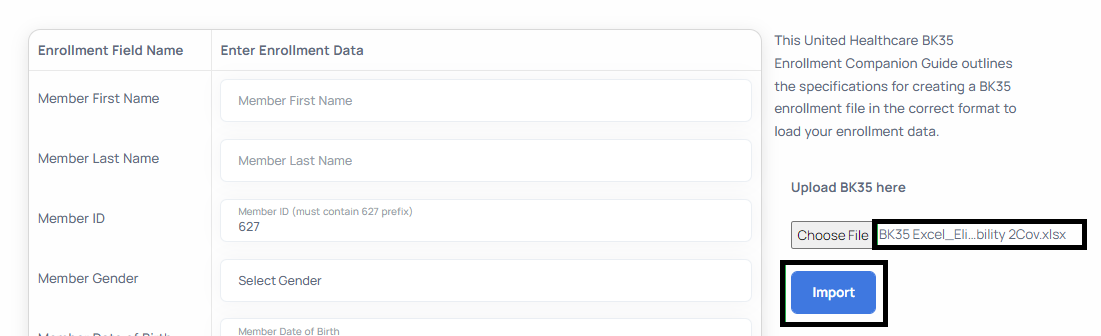
- When the container field is populated as depicted below, click the import button to upload the enrollment data and to submit the file for processing.
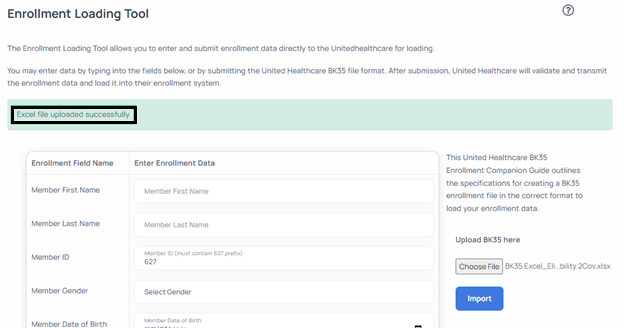
- The screen will depict a success message indicating that your file has been submitted successfully as depicted below.
ELECTRONIC ELIGIBILITY LAYOUT - FULL FILE 1X LOAD SPREADSHEET
| COLUMN | LGTH | DATA ELEMENT | DESCRIPTION | REQUIRED / OPTIONAL / SITUATIONAL |
|---|---|---|---|---|
| A | A (8) | Record Control Data | Valid Value: BEK0035 | R |
| B | A (3) | Filler | Reserved - Default Spaces | R |
| C | A (1) | Member Code | Identifies member: A = Employee B = Spouse C = Dependent |
R |
| D | N(2) | Filler | Hidden Column - Do not delete Reserved - Default Spaces (sequence nbr not used for 1x loads) |
|
| E | A (9) | Filler | Hidden Column - Do not delete | |
| F | A (20) | Last Name | Last Name | R |
| G | A (14) | First Name | First Name | R |
| H | A (1) | Middle Initial | Middle Initial - Default Spaces | O |
| I | A (3) | Name Qualifier | Valid Values: SR, JR, II, III, IV, MD - default spaces | O |
| J | A (35) | Street Address | Participant only | R |
| K | A (35) | Street Address | Participant only - Default Spaces | O |
| L | A (20) | City | Participant only | R |
| M | A (2) | State | State Code Abbreviation - Participant only | R |
| N | A (2) | Country | Foreign countries only, ANSI Code - Participant only - Default Spaces | O |
| O | A (8) | Filler | Hidden Column - Do not delete Default Spaces | |
| P | N (9) | Zip Code | Participant only | R |
| Q | N (8) | Date of Birth | Participant birth Spouse birth Dependent birth Format is CCYYMMDD |
R |
| R | A (1) | Gender | Valid Values: M = Male F = Female |
R |
| S | A (1) | Individual Relationship Code | Participant Record: Marital Status Valid Values: S = Single M = Married U = Unknown or Domestic Partner Spouse Record: Valid Values: 2 = Spouse T = Deceased Spouse Dependent Record: Valid Values: 3 = Child |
R |
| T | N (8) | Group Number | Identifies Customer - Will provide - see Account Structure spreadsheet |
R |
| U | N (3) | Participant Location | Identifies geographical location of participant - Will provide - see Account Structure spreadsheet |
R |
| V | A (1) | Work Status | Participant only: Valid Values: A = Active T = Terminated D = Deceased R = Retired S = Surviving Spouse/Child |
R |
| W | A (2) | Work State | Participant only: State code abbreviation Recommended: Copy the Address State from Column M |
R |
| X | N (8) | Original Hire Date | The original hire date is required for stop loss. If an account has dental, this date is used to apply waiting periods.
If the account applies pre-existing, this date is used to determine if the employee has met their pre-existing time limit and is eligible for full benefit consideration for all conditions. Format is CCYYMMDD Default Zeroes |
O |
| Y | N (8) | Filler | Hidden Column - Do not delete Reserved Default Zeroes |
|
| Z | N (9) | Filler | Hidden Column - Do not delete | |
| AA | A (1) | Filler | Hidden Column - Do not delete | |
| AB | N (1) | Filler | Hidden Column - Do not delete
Reserved Default Zeroes |
|
| AC | A (9) | Filler | Hidden Column - Do not delete | |
| AD | A (4) | Filler | Hidden Column - Do not delete
Reserved Default Spaces |
|
| Coverage 1 |
||||
| AE | A (1) | Line Description Code | Identifies product covered Valid Values: H = Health |
R |
| AF | N (12) | Plan/Contract Number | Identifies coverage line - Will provide - see Account Structure spreadsheet |
R |
| AG | N (8) | Effective Date | Effective date of coverage Format is CCYYMMDD If we are paying run-in claims, enter effective date of run-in or later |
R |
| AH | N (8) | Termination Date | Date coverage terminates Format is CCYYMMDD If we are paying run-in claims, enter term date. |
S |
| AI | A (3) | Class Code | Classification of Participant Will provide - see Account Structure spreadsheet |
R |
| AJ | N (1) | Coverage Type | Valid Values: 1 = Participant only 2 = Dependent only 3 = Family Two Tier = 1,3 Three Tier = 1, 3, 4 Four Tier = 1, 3, 5, 6 |
R |
| Coverage 2 |
||||
| AK | A (1) | Line Description Code | Identifies product covered Valid Values: D = Dental |
R |
| AL | N (12) | Plan/Contract Number | Identifies coverage line - Will provide - see Account Structure spreadsheet |
|
| AM | N (8) | Effective Date | Effective date of coverage Format is CCYYMMDD |
|
| AN | N (8) | Termination Date | Date coverage terminates Format is CCYYMMDD |
|
| AO | A (3) | Class Code | Classification of Participant Will provide - see Account Structure spreadsheet |
|
| AP | N (1) | Coverage Type | Valid Values: 1 = Participant only 2 = Dependent only 3 = Family Two Tier = 1,3 Three Tier = 1, 3, 4 Four Tier = 1, 3, 5, 6 |
|
| AQ | N (10) | Not in Use | Hidden Column - Do not delete | O |
| AR | N (8) | Not in Use | Hidden Column - Do not delete | S |
| AS | N (8) | Not in Use | Hidden Column - Do not delete | S |
| AT | N (10) | Not in Use | Hidden Column - Do not delete | O |
| AU | N (8) | Retirement Date | Retirement Date (if applicable) Format is CCYYMMDD |
S |
| AV | A (15) | Customer Rptg Field 1 | Participant only. Customer Reporting Default Spaces |
S |
| AW | A (15) | Customer Rptg Field 2 | Participant only. Customer Reporting Default Spaces |
S |
| AX | A (15) | Customer Rptg Field 3 | Participants only. Customer Reporting Default Spaces |
S |
| AY | A (15) | Customer Rptg Field 4 | Participants only. Customer Reporting Default Spaces |
S |
| AZ | A (15) | Customer Rptg Field 5 | Participants only. Customer Reporting Default Spaces |
S |
| BA | A (15) | Customer Rptg Field 6 | Participants only. Customer Reporting Default Spaces |
S |
| BB | A (15) | Customer Rptg Field 7 | Participants only. Customer Reporting Default Spaces |
S |
| Coordination of Benefits Information 1 |
||||
| BC | A (1) | COB Line Code | Indicates Line of Other Insurance Coverage Valid values: H = Health coverage D = Dental coverage B = Both Health & Dental |
O |
| BD | A (1) | COB Indicator | Indicates whether there is Other Insurance Cov. Valid values: S = Single coverage F = Family coverage Y = Yes (if S/F not avail) N = None U = Unknown |
O |
| BE | A (1) | COB Level | Indicates level of Other Insurance coverage
Valid values: P = Primary S = Secondary T = Tertiary U = Unknown |
O |
| BF | A (20) | COB Carrier Name | Name of Carrier for Other Insurance | O |
| BG | N (8) | COB Effective Date | Effective Date for Other Insurance Coverage Format is CCYYMMDD |
O |
| BH | N (8) | COB Termination Date | Termination Date for Other Insurance Coverage Format is CCYYMMDD |
O |
| BI | N(9) | Employee ID | 9 digit Member ID (UHC Member ID) | S |
| BJ | A/N (62) | Not in Use | Hidden Column - Do not delete | S |
| BK | N (10) | Not in Use | Hidden Column - Do not delete | O |
| BL | A/N (30) | Other ID | Other ID (if applicable) | S |
User Management
Accessing User Management
Users with a Super Admin role will have access to the User Management feature that will allow them limited control over the other users under their class code. If enabled, this option will only be available by clicking on User Management from the landing page as depicted below.
- Once you have clicked on the User Management option, the screen depicted below will load. This screen will list all active portal users affiliated with your particular class code. As a Super Admin user, you can use this functionality to perform any of the actions below.
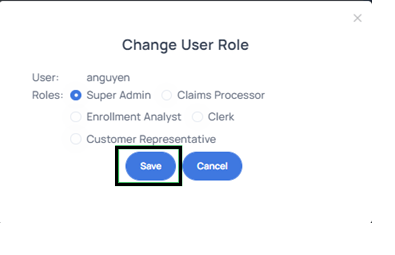
- Clicking on the Edit Role button for a user will display the pop-up box below. You can change the user's role by simply selecting a new role and clicking save as depicted below.
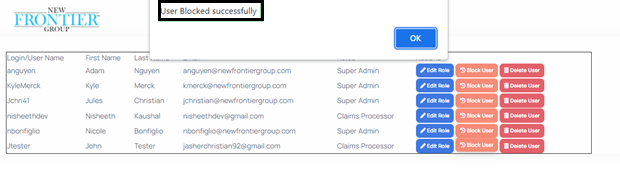
- Clicking on the block user button will display the pop-up box depicted below. The user will be blocked from logging into the portal until a Super Admin uses this functionality to unblock the user.
- Clicking on the Delete User option will permanently deactivate the user. This should only be done for users who have changed roles or have left the organization.